Children born with congenital heart defects will live their entire life without a cure. There isn’t a single medication, treatment, or surgery that will ever fix their hearts. Over fifty percent of children born with a congenital heart defect will have at least one invasive, open-heart surgery in order to repair the defect(s), but their hearts will never be fixed. Across the globe approximately, 10% of all children diagnosed with a congenital heart defect will be deemed uncorrectable through repair surgeries and procedures, and the child will be listed for a heart transplant.
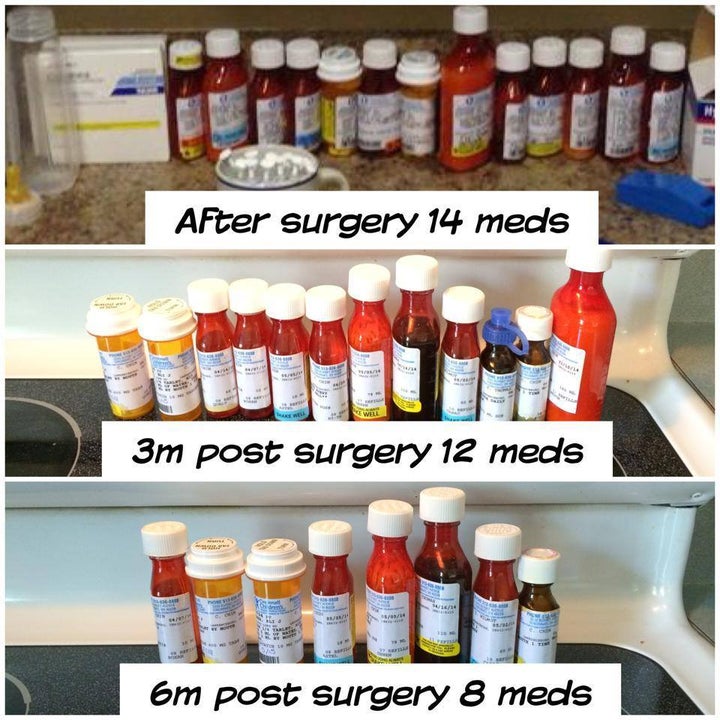
Heart transplants are not a cure, in fact, it takes a significant amount more medication, treatments, and procedures to maintain the hero heart, than many children both with congenital heart defects take on a regular basis for their biological heart. Should the child survive open heart surgery, have a successful transplant, and the donor heart remains viable post-surgically, they will have to take multiple medications throughout each day. Some of these medications include, but are not limited by any means to: cyclosporine, tacrolimus, mycophenolate mofetil, steroids (prednisone or methylprednisolone), azathioprine, and thymoglobulin. Even with all the advances in modern technology, the body will never 100% accept the donor heart as its own.
In fact, it is the very hope that each medication will continue to do work within specific parameters in order to keep the new heart, and each child, alive. Children that receive heart transplants are also not guaranteed to survive past ten years on average, but fifteen to twenty years, at best, before needing another transplant. The survival rate of pediatric heart transplant recipients is 61% at the ten year mark and steadily declines from there. The International Society for Heart and Lung Transportation 2016 slides provides this information and many more details on pediatric heart transplant statistics. While every hospital hinges on their survival rates, that very depending on the facility, each family seeks to provide the best quality of life they can, regardless of the survival time.
They know that with each fever, infection, and flu season comes with the chance of a battery of testing, a hospital admission to rule-out rejection, or death. Within my limited sphere of influence through Gracie’s Gowns, we have seen many children pass away, not from their diagnosis, or complications related to their diagnosis, but because they caught a virus, the flu, or acquired an systemic infection their bodies could not fight, even with the strongest of antibiotics or antivirals available.
Long-term complications can arise as well, and may not even happen until months or years post-transplant. As a result of the chronic use of immunosuppressive medications to prevent rejection, pediatric heart transplant recipients can develop cancer, kidney damage that would require a second organ transplant, and high blood pressure. In addition to those concerns, is the development of coronary artery disease that could result in their child’s death, or the need for another heart transplant.
Life becomes a delicate balancing act of appointments, medication schedules, therapies, evaluations, blood draws, and spending time as a family, attempting to accept the new normal the best one can. During the immediate time post-transplant through the first year, they struggle with the desire to physically put their in a bubble to protect them from just about everything and everyone...and yet still allow their child to just be a kid. While many children will return back to school, to activities, to their normal level of function within time, there are still restrictions on what they can and cannot do for the sake of helping their donor heart last beyond that ten year mark.
So to the well-intended, but grossly under-educated follower who decided that once children receive their hero heart, they were no longer considered chronically-ill or in need of constant medical care...I hope we helped you understand just a little bit more about what these families still have to go through post-transplant.