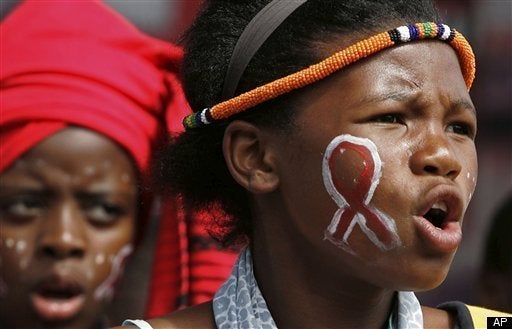
This piece is part of a series of blogs by leading NGOs to call attention to a range of issues that should be raised at the G8 summit at Camp David in rural Maryland from May 18-19.
I first met Nasanta* several years ago when she was brought by her grandmother to our free AIDS clinic after the death of her mother. A bright, engaging 13-year-old Zambian girl living with HIV, she had come from a city six hours away to live with her impoverished grandmother in our remote, rural district; and she came with a heartrending story.
Nasanta's father had abandoned them after her mother had become sick with AIDS. Her mother decided to have Nasanta tested, and the positive result put her in a position no mother should have to face. Although the government was making "low-cost" antiretroviral (ARV) drugs available with the help of Western donors, Nasanta's mother knew she could not afford the cost of these drugs for both of them. So, she decided to forgo the drugs in order to provide them for her daughter. About a year later, she made the supreme sacrifice and Nasanta found herself orphaned. Fortunately, when Nasanta came to our mission hospital, we had recently begun providing ARVs free of charge with funds from the U.S. government through a secular and faith-based consortium called AIDS Relief. With the medicine, Nasanta was able to remain healthy.
It is impossible to overstate the impact of providing ARVs without charge. As a doctor practicing in Africa, I have seen the AIDS pandemic unfold. I remember the hopelessness of each diagnosis as all we could do at first was treat the patient's opportunistic infections. "Low-cost" ARVs improved the situation for some. But the astounding transformation came when the U.S. government's PEPFAR fund (U.S. President's Emergency Plan for AIDS Relief) and the Global Fund (to treat AIDS, TB and Malaria) made it possible to provide ARVs at no charge. For the first time in the history of the pandemic, we saw real hope. I have witnessed the nearly dead restored to healthy life, children return to school, and economic productivity return to villages. I have witnessed the spread of HIV slow down as progress has been made in identifying effective prevention strategies.
When we entered Zambia in 1997, almost one in five adults was already infected with HIV. As of 2009, the prevalence rate had declined by a third. In Kenya, HIV prevalence in adults peaked in 2001 at 15 percent. A mere eight years later it had dropped to just 6.3 percent. Similar declines have been seen in the number of HIV-infected babies born to positive mothers as testing and ARVs have become a routine part of prenatal care. This has generated profound goodwill among Africans toward America.
But all this progress is now being threatened. The economic downturn has resulted in cutbacks in funding for AIDS. Defaults on promises made to the Global Fund forced the cancellation of the entire Round 11 grants, halted the implementation of program scale-ups and blocked new enrollments into ongoing programs.
At Kijabe Hospital where I work, its PEPFAR-funded program has been recognized as a "best practices" program in Kenya. Yet in 2010, it was notified of a 20 percent cut in funding. In order to continue providing essential ARVs to over 5000 active clients, it was forced to cut back on its community-based activities. Treatment default rates rose as community workers could no longer follow up with patients, followed later by increasing mortality rates.
The U.S. government is focusing its aid on helping governments in hardest-hit countries to strengthen their national health systems. But in the process, the faith-based hospitals and clinics, which provide 40 to 70 percent of health services in rural Africa, are finding themselves being left out. This is unfortunate, as the faith-based sector holds great potential for contributing to community-based prevention efforts, providing care and treatment for people living with HIV, caring for orphans and vulnerable children, and advocating for the rights of those affected by HIV and AIDS.
Today we are closer than we have ever been to defeating the AIDS pandemic, so close that UNAIDS has set a goal of "zero new HIV infections, zero discrimination and zero AIDS-related deaths." But with an estimated 34 million people infected as of 2010, we are also on the edge of disaster with the very real possibility that much of the hard-won gains of the past several years may slip through our fingers.
The G8 and other donor nations must not yield to the pressures to back down. They must follow through on commitments and enable the continued scaling up of access to diagnosis, care and treatment of people living with HIV and the expansion of prevention efforts, including behavior change. And if they want more bang for their buck, they should include the faith-based sector as a strategic partner, for the sake of Nasanta and her mother and the millions more mothers, fathers, sons and daughters affected by HIV and AIDS.
*Nasanta's name has been changed to protect her privacy.
Read more G8 news and blogs on HuffPost's G8 big news page.