
Elizabeth* always thought she just wasn’t really into sex.
It was something she enjoyed but never something she initiated. She was attracted to people but rarely felt aroused. When she was in her early 20s, conversations with friends made her realize that her experiences of sex were much fewer and less enthusiastic than a lot of other people her age.
“I just knew that maybe I was missing that urge,” Elizabeth, who lives in southern Ontario, told HuffPost Canada.
Elizabeth says she’s been taking antidepressants since she was 15 — before she started having sex. Now in her early 30s, she’s come to realize that there might be a connection between her low sex drive and the meds she needs to keep her depression in check.
After long conversations with her partner, and under the supervision of a doctor, she’s decided to switch medications. If other parts of her life start to suffer, she has no problem switching back, she said. But she wants to experience something she feels she’s never really had: a sex life unclouded by side effects. She’s optimistic that she might even discover a whole new relationship to physical intimacy.

It’s all too common a problem
Carlyle Jansen, a sex coach and educator for more than two decades who founded Toronto’s Good For Her sex shop, says she encounters stories like Elizabeth’s often.
“The number of people who weren’t told by their doctor that SSRIs tend to affect ability of orgasm!” Jansen told HuffPost Canada. “I don’t know why doctors don’t mention that.”
SSRIs, or selective serotonin reuptake inhibitors, are the most commonly-prescribed form of antidepressant, according to the Mayo Clinic. They work by increasing the brain’s supply of serotonin, a neurotransmitter that can — to simplify complex brain chemistry — increase happiness. Some very common SSRIs include Prozac, Paxil, Zoloft, and Lexapro.
The long lists of potential side effects that accompany many medications are common enough to have become a trope of hacky comedy. And many of the medications people rely on, sometimes for temporary relief and sometimes to control long-term conditions, can truly interfere with a person’s sex life.
One of the biggies, for people of all genders, is antidepressants. Depression can kill libido — but so can many of the meds, especially SSRIs, prescribed to treat the condition. They can make it more difficult for men to get or sustain erections and make it hard to achieve orgasm.
One of Jansen’s clients told her that, for someone finally interested in sex after a bout of depression, not being able to climax feels like “you’re getting all dressed up, and you’re excited, but then you’re at the party and you can’t enjoy yourself.”
But there are several other drugs, used to treat all kinds of different issues, that can also cause sexual problems. Some birth control methods, including the pill, hormonal IUDs, implants, and injections can lower sex drive, which seems counter-intuitive given that they’re designed so people can have sex safely.
Opioids for pain, antihypertensives for people with high blood pressure, hormone therapy, and antipsychotic meds can all affect sex drive and arousal for all genders. Erection and ejaculation are reflexes, so anything that interferes — like antispasmodic or nerve pain meds — can make those acts more difficult.
Even simple antihistamines like Benadryl can cause erectile dysfunction as well as dry mouth, nose, throat — and without putting too fine a point on it, dries out vaginas, too.
“Some people can go down a rabbit hole about what this all means, where really all it means is: I need medication.”
- Carlyle Jensen, sex educator
Too many people are afraid to bring it up with their doctors
These side effects can be hard for patients to talk about, because both sex and medication carry a lot of stigma, Jansen said. And that can lead to further problems.
“I think sexual side effects are one of the main reasons that people discontinue medication,” University of British Columbia professor and sexual medicine physician Dr. Stacy Elliott told HuffPost Canada.
People with sexual concerns are often too scared to bring them up. They tend to “wait for the doctor or the health-care professional to ask — and health-care professionals are not good at that,” Elliott said.
“We’re really pushing in medical school and residences to make sure that you ask about sex, bladder, bowel. And for some reason, health-care professionals are more comfortable with bladder and bowel than they are sex.”
It can be especially difficult for people who identify as men, who are often subject to intense social pressure about their virility. One study of cisgender men aged 50-76 living in New York state found that only about a third of the participants who experienced erectile dysfunction for any reason sought treatment for it, usually because they had received misinformation about it or else because they were embarrassed.
Men are also less likely than women to seek help for depression due to “the problematic impact of conformity to traditional masculine norms,” another study put it.
In other words, there’s still enormous social pressure preventing a lot of men from seeking help for sexual problems. This is true to Elliott’s experience in urology, she said. “Women are, I think, much more comfortable talking about sexual or reproductive organs, because they’ve had to deal with them every month,” she said. “The whole genital area gets talked about more than men.”
Beyond the obvious problem — people might go off meds that are helping them, physically or mentally, in really significant ways — men who aren’t comfortable talking to their doctors about sex might actually miss important signals about their health.
“When a man is coming in for a blood-pressure check, not many family docs would ask, ‘How are your erections?’” Elliott said. But difficulty with erections can actually be an early indicator that something might be wrong with cardiovascular health.
Watch: 10 things that can cause a low sex drive. Story continues after video.
It’s common for people whose sex life is impacted by medication to go down a “rabbit hole about what this all means,” Jansen said. They might wonder why they can’t satisfy their partners or what’s wrong with their bodies. But really, she said, “All it means is: I need medication. It’s impacting me. How do I get around it?”
Sometimes it means switching drugs
Marla,* a Toronto resident in her late 20s who’s been on antidepressants for nearly two years, said she was nervous bringing the topic up to anyone.
She started taking Prozac a few months before meeting her current boyfriend. The first time they had sex, “my body didn’t react the way I was expecting it to and the way it had in the past,” she told HuffPost. Even though she was aroused, she said, she wasn’t getting wet.
She told her boyfriend what was going on. It was earlier in the relationship than she probably would have told him she was on antidepressants, but he was supportive.
When she told her doctor she wanted to switch medications, “I was super nervous, even though my doctor is a woman and she’s young and she’s open-minded,” Marla said. “I’m just not used to talking about this stuff to anyone.”
She switched from an SSRI to an SNRI (serotonin-norepinephrine reuptake Inhibitor), a class of antidepressant generally thought to have fewer sexual side effects — though according to Elliott that’s difficult to know for sure. It was an easy transition for Marla, since she was still new to antidepressants, and the new drug worked for her.

But for many people, changing drugs isn’t as easy or convenient. Back when Elizabeth was first prescribed meds years ago, she had to try several different kinds before she landed on the one that worked for her. One of them made her gain a lot of weight; another made her depression even worse — a confusing side effect of many antidepressants.
And now, as she tapers off one drug and switches to another under a strict schedule prescribed by her doctor, she’s experiencing some withdrawal symptoms. She’s tired a lot, and she’s had some mood swings.
She counts out her pills every day, knowing there are big risks if she strays from her complicated schedule: her depression could come back, she might get shakes or electric shock-esque “brain zaps,” or she might start acting in a totally unpredictable way. But if this is what has to be done to treat her depression and give her a real sex life, “it seems like a reasonable tradeoff,” she said.
The good news is that there are lots of strategies to get around drug-induced libido problems, Jansen said. First of all, talk to your doctor to see whether there are any other meds you could take. It’s important never to go off medication, particularly antidepressants, without talking to your doctor first. So-called “drug holidays” only work for specific kinds of meds, Elliott said, and should never be attempted without a doctor’s supervision.
If that’s not an option, try to focus on your body and how it feels to “work with the realities of your life,” Jansen said. Is there a time of day when your meds most affect you? Some drugs are rapid-acting, so both the intended effect and the side effects will be most present immediately after you take them. Maybe morning sex, before you take your meds, will be more successful for you. Is there a kind of sex that’s more painful for you? Switch it up to something else.
She also suggests trying different sex toys. For women or trans people with vaginas who have trouble reaching orgasm, maybe a vibrator will help. There are also toys designed to be enjoyed by a non-erect penis; Jansen suggests a brand called Hot Octopuss (link NSFW, naturally).
“The most successful relationships are not the ones that have the most orgasms,” she said. “It’s people who are creative, who take risks, who are being vulnerable, who are honest and genuine with each other and who are pleasant with each other. That can happen with or without orgasm. That can happen with or without intercourse.”
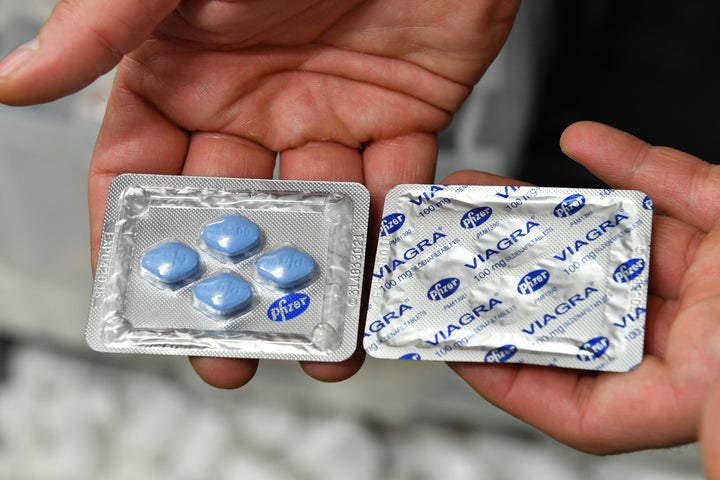
Cis men have the option of turning to other medication. Drugs like Viagra, Cialis or Levitra won’t create erections, but they can enhance them, Elliott explained.
There’s no such option for women. One American company did try to create a drug intended to increase women’s arousal. But flibanserin, sold under the brand name Addyi, isn’t a great solution, according to Elliott. Its use is extremely limited, as it can only be used by pre-menopausal women who don’t drink alcohol and — in most cases — don’t take other meds. The drug hasn’t been approved for use in Canada, and Elliott doubts that will happen any time soon.
For most people, sex is an important part of a romantic relationship. The comfort you develop talking to your doctor about things that are embarrassing, as well as the skills you develop talking to your partner about your needs, are guaranteed to serve you well later in life, Jansen said.
Having open and honest conversations about sex with a partner probably feels awkward at first, but it’s worth pushing through that to get to a place where your needs are understood.
Everyone’s sex life changes over time. Maybe a needed drug will decrease your libido. Maybe you’ll suffer an injury. Maybe you or your partner will have a baby. You’ll definitely both age.
“Whatever goes on in our lives, things are going to change,” Jansen said. “We have to adapt.”
*Names have been changed at our sources’ request to protect their privacy.
Also on HuffPost: