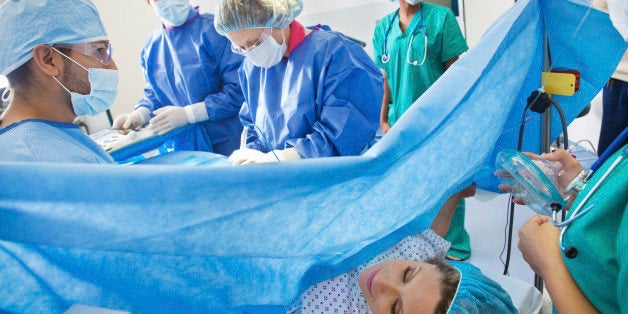
Pregnant American women give birth via caesarean section at more than double the rate the World Health Organization recommends.
Outcomes for both mother and baby improve as a country’s rate of caesarean sections tops 10 percent, according to a WHO report released Friday. But there's no evidence that health care quality continues to improve once a country's rate exceeds 15 percent, WHO said.
The rate of caesarean section births in the U.S. was 32.7 percent in 2013 -- well above the “medically necessary” target of 10 percent to 15 percent that WHO says is ideal. Germany and Italy have similarly high rates -- 32 percent and 38 percent, respectively -- while low-income countries like Afghanistan and Kenya hadn't yet reached 10 percent, according to data from 2011. Brazil, notorious for high caesarean rates, tops the list at 52 percent.
Caesarean births, or c-sections, are an abdominal surgery in which doctors slice through skin, the abdominal wall, muscle and the uterus to delivery a baby. When they're medically necessary, c-sections can help save the life of mother and child during complications, like breech birth and umbilical cord prolapse (when the cord slips into the vagina). In addition, the baby may be too big to safely pass through the birth canal, or the baby could be in distress.
Medically unnecessary reasons for a c-section include planning a due date around work or travel plans, or even a doctor’s schedule -- in effect transforming a notoriously inefficient process (healthy labor can take up to 24 hours to delivery a baby) to an operation of less than two hours.
Like any other major surgery, c-sections can have complications, like damage to other organs, internal bleeding, blood clots or infection. Recovery after a c-section is typically longer than that of a vaginal birth. Moms who have c-sections may experience as much as six weeks of post-operation pain and bleeding, versus bleeding and vaginal discharge for two to four weeks after a vaginal birth. Finally, women who have a c-section for their first baby will face risks for subsequent pregnancies, like a higher chance of the placenta implanting or growing abnormally, or uterine rupture along the site of the scar. If they’re at high risk for complications, U.S. mothers will probably need to have the operation for all subsequent births, according to the American Congress of Obestritians and Gynecologists’ recommendations.
Dr. Linda Szymanski, the medical director of labor and delivery at Johns Hopkins Hospital, performs elective c-sections for a small number of patients who request them. Some may simply want to time their delivery around other life events, but others may have experienced some kind of sexual trauma in the past that makes them feel they cannot psychologically handle labor or a vaginal delivery, she explained. Others may worry about vaginal trauma or exacerbating urinary incontinence, even though their fears may be unfounded.
Szymanksi said in an email to HuffPost that the hope is that an elective c-section is chosen after “thoughtful and complete counseling,” and conducted by a doctor who is comfortable performing the surgery under those conditions.
"Truly, the number or women who request elective cesareans is relatively low (perhaps 2-3%),” wrote Szymanksi. "When women request this, it is critical for them to sit down with their doctor and have a frank discussion about the potential risks involved in having a c-section.”
While Szymanski said she believes most doctors think c-sections should be reserved for those who need it medically, she thinks it's unrealistic to try to push the American rate below 15 percent.
"I think it is important to realize that the WHO is speaking about international health care, and includes recommendations for countries with high rates of pregnancy complications and maternal deaths,” said Szymanski. "The bottom line is that I think it is difficult to apply the WHO recommendation to the United States.”
Dr. Patricia Robertson, a practicing OB/GYN and professor of obstetrics, gynecology and reproductive sciences at University of California, San Francisco, said she thinks the U.S. can reach the WHO target. For instance, San Francisco General Hospital, which is a public teaching hospital connected with UCSF, has a c-section rate for first-time moms of 10 percent for 2013, well below the California average of 17.1 percent that year.
A combination of structural policies, including paying doctors a salary instead of paying them per service, the use of nurse-midwives as primary caregivers and an obsession with evidence-based medicine, contribute to the hospital's low c-section rates, said Robertson.
A 2015 study that compared the care of traditional private practice doctors to midwives or laborists (salaried doctors who work by shift) within the same community hospital found that women laboring with a traditional doctor were significantly more likely to have a c-section than women laboring with a midwife or a laborist (31.6 percent vs. 17.3 percent). Because they’re salaried, laborists have no incentive to push for expensive c-sections, and nurse-midwives tend to be more patient and supportive, Robertson said.
Patient and family education and mental health are also major components of keeping rates low.
“It is very important for women to realize that their obstetrical outcome is the most important priority, not the person who is there at delivery,” said Robertson. “These days we work in teams, so that there are smooth transitions of care that do not depend on the presences of their own obstetrician -- although if that works without increasing their risk of a caesarean section, that is wonderful for both the patient and the obstetrician."
CORRECTION: A previous version of this story incorrectly linked Dr. Patricia Robertson to University of San Francisco. She works at the University of California, San Francisco. We regret the error.
