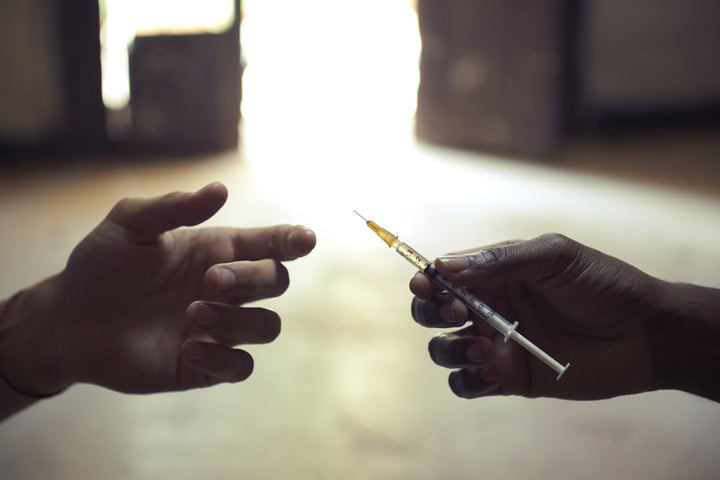
Washington, D.C. has a higher AIDS diagnosis rate than any U.S. state, with about 2.4 percent of residents living with HIV/AIDS. Just over 14 percent of those cases are linked to injection drug use.
But until 2007, there was a federal ban on using D.C.'s municipal funds for needle exchange programs, an outreach technique that reduces disease spread and can channel vital health and addiction services to drug users. When Congress lifted the ban, public health scientists were eager to see if needle exchanges would stem the tide of new HIV cases in the district.
Thanks to a new study that followed the first two years of such needle exchange programs in D.C., the verdict is in: By funding the exchanges, lawmakers helped avert at least 120 new HIV cases in the District in the first 24 months, saving an estimated $44 million in lifetime costs for HIV/AIDS care.
Currently, only 16 states and Washington, D.C. explicitly authorize needle exchange programs, according to April 2015 data from LawAtlas. But research consistantly shows that providing clean needles to drug users reduces infectious disesase and, despite claims to the contrary, doesn't "encourage" drug addiction.
"A lot of policymakers are caught up in that belief system without looking at the evidence,” said lead researcher Monica Ruiz of George Washington University’s Milken Institute School of Public Health. But, she said, this latest study provides clear evidence that setting aside such biases in favor of evidence-based policies can save lives -- and help reduce an unnecessary health care burden.
How needle exchanges work
Injection drug users have a higher risk of contracting blood-borne diseases like HIV and hepatitis B and C because the disease can be transferred from an infected person to a new person if they use the same needle. In the U.S., injection drug users represent eight percent of all new HIV infections and 16 percent of new hepatitis B infections. Globally, about 90 percent of all new hepatitis C infections are linked to injection drug use.
Cleaning needles and other drug paraphernalia does not completely remove these pathogens. That's why new, sterile syringes are the safest way to inject drugs, although drug abuse in general is also linked to riskier lifestyle behaviors like sex without a condom and sex work — behaviors that also increase risk of HIV and hepatitis.
Past research from other areas of the country has linked access to clean syringes to huge reductions in both hepatitis B and C infections and HIV infections. In addition to providing access to clean equipment, experts say, these programs are important points of contact where medical personnel can refer drug users to other services that may help address addiction and health.
“States can't afford to wait for the next HIV outbreak; they need to start setting up needle exchange programs today.”
- Daniel Raymond, policy director for the Harm Reduction Coalition
Analyzing D.C.'s program
Ruiz used a statistical model to predict how many injection drug-associated HIV cases District residents would have acquired if the district's needle exchange program had never been created.
In this alternate universe, D.C. would have seen a total of 296 injection drug-related HIV cases in the first two years. In reality, the district counted only 176, which means that at least 120 people dodged an HIV diagnosis as a result of the needle exchange policy, according to the researcher's calculations.
In addition to saving 120 people from an HIV diagnosis, the program, which cost the city $1.3 million over two years, saved an estimated $44.3 million in lifetime HIV costs those 120 patients would likely have incurred. It also opened the door for public health workers to reach at-risk people with other interventions, like distributing condoms and HIV tests. It connected 321 people to substance abuse treatment.
Ruiz's analysis is unique, because while other research has measured the effects of a needle exchange program before and after it was implemented, her study assesses the impact of how policy, and investing local funds, changed the rates of new HIV contractions in D.C. The District did have an independently funded needle exchange program before Congress lifted the ban on using municipal money, but once the ban was lifted, D.C. was able to invest a lot more to enhance and expand its services.
Indiana's example
The human cost of not having a needle exchange program became clear in Indiana’s Scott County, which saw an explosion of HIV cases tied to intravenous drug use. The small county, which has just under 24,000 residents, had never seen more than five HIV cases a year, but in 2015 that number is so far up to 177. In response to the crisis -- and despite a long-held stand against needle exhange programs -- Gov. Mike Pence (R) established temporary service in the county. Ruiz praised Pence for his “tremendous” leadership on the issue, as well as his ability to set aside his personal bias in favor of evidence-based programs that have been shown to prevent the spread of HIV.
"He said, 'Regardless of what I think, this is what the people need,'” said Ruiz. "I hope other policy makers take that lead, because there are a lot of states who could use that more advanced thinking."
But Daniel Raymond, policy director for the Harm Reduction Coalition, said if states wait until a disease outbreak to start a needle exchange program, it’s already too late.
"States can't afford to wait for the next HIV outbreak; they need to start setting up needle exchange programs today,” Raymond said. And in fact, states don’t have as difficult a path as D.C. did to lift the ban. Because the city is governed by Congress, the syringe exchange ban could only be lifted with a new national law, signed by sitting President George W. Bush (R).
Other states can learn a lot from this bipartisan effort, said Greg Millett, policy director for amfAR: The Foundation For AIDS Research.
"The fact is that this policy change in Washington, D.C. is because of President George W. Bush signing this 2008 financial services bill, [which went] through a Democratic Congress,” said Millett. “It’s led to some really fantastic results for injection drug users, and I think it’s certainly instructive."
Drug use is the 'canary in the coal mine'
Rising rates of prescription opiate abuse and heroin use in certain parts of the country are the “canary in the coal mine” that indicates if a state or jurisdiction should set up a needle exchange program, Ruiz said.
“If these people are using these drugs, there’s a good possibility they’re injecting, and there’s a good possibility that they’re serious users,” she explained. "And there’s a good possibility that they’re going to need things like needle exchange programs."
Ruiz published her study in the journal AIDS and Behavior.
Also on HuffPost:
