The CDC released news this week that opioid prescriptions have declined since 2010 ― a welcome and positive step. It means that doctors are being more careful and conservative before they write a prescription for opiate pain medications like hydrocodone or oxycodone. Their well-intended dispensing of these powerful narcotics historically was what in large part caused today’s opioid crisis to explode, and this indicates a course correction of sorts.
But the news is only part of the story and needs to be taken in the context of the greater, more dangerous and terrifying reality: if you stop prescribing an opioid to a person who is dependent, they will have to either medically treat their opioid addiction or use illicit street drugs like heroin to satisfy the overwhelming cravings that are the pathological marker of the disease.
I applaud the medical community for having done a good thing in turning the tide on the initiation of potential addiction patient in the future. However, for our communities, we may have started a ticking time bomb at the same time and it has to be acknowledged and dealt with.
First, let me be very clear. I was as pleased as anyone to see that opioid prescriptions had dropped. Current data shows that a significant portion of today’s opiate addicts, including heroin, got their first opiate exposure in the form of a well-intended medically supervised prescription. I cannot tell you how many suffering people I have spoken with, who were in the horrific throes of heroin withdrawal, or had lost a loved one from an overdose. What has been so telling about the opioid crisis is that the vast majority of people who struggle with addiction, most likely would never have encountered, let alone sought out, actual heroin – it was the farthest thing from their thinking and life experience.
The Surgeon General’s Report on Alcohol, Drugs and Health estimated 80 percent of heroin addicts started their opioid abuse with a prescription. This vicious cycle has been well-documented and well-studied, and I applaud CDC Commissioner, Tom Frieden, who in 2016 bravely wrote new guidelines for opioid prescriptions as well as a letter to every primary care physician urging restraint and emphasizing the risks with these medications. But I also need to set off an alarm, because this has created a desperately dangerous scenario for the 2.5 million people suffering with opioid addiction. You can cut the engine on a speedboat, but the boat will still sail forward for some time before coming to a stop, and that’s where we are in the crisis. We as a nation need to ensure that we have the power and the foresight to reverse our course with these patients before it’s too late for many of these individuals.
While the quantity of prescriptions has gone down, deaths from overdoses have drastically risen. In the United States, we are now over 50,000 deaths per year. But this sad and troubling fact is easy to explain. There are two main reasons that we are seeing a rising body count. The first is the prevalence of Fentanyl and Carfentanyl in street heroin. In many cases, unbeknownst to the buyer, the heroin they buy can be 100 times stronger and kill them instantly. The supply chain from the drug cartels, to the street corner dealer, don’t exactly have quality assurance provisions like a pharmacy would, nor do any of the operators even care. Therefore, each time a person struggling with addiction buys heroin they are playing Russian Roulette.
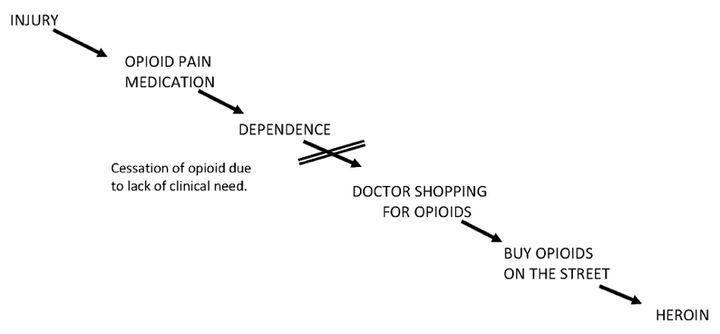
The second reason is that if a patient has a prescription for an opioid to which they have become dependent, stopping the prescription will not stop their cravings or their use of opioids. On the contrary, it will set off a potentially deadly spiral of addiction pathology and it is medically irresponsible to simply stop writing scripts without a plan for that patient to undergo care. Take a look at the illustration below to see the typical path a medical patient may take.
Let’s all recognize that none of these patients choose to become addicted to their medications. Many were simply following the appropriate directions given to them by their medical care givers. Its their biology driving this process for many of them. Withdrawal treatment is necessary and should be discussed without shame and with great urgency. A significant part of our practice, in my organization, is receiving patients from leading pain clinics who are clinically done with their treatment for injury but have become dependent on their prescribed opiates. Part of eliminating the shame and stigma around the idea of addiction, could be to simply rename it “opioid cessation.” This is a non-judgmental term with no baggage and it worked combatting the public health problems of tobacco.
We need to realize that currently there are millions of people who woke up this morning, whose sole goal and need today is to satisfy an opioid craving because they are medically unable to do otherwise. Their biological need is driving this, and every one of them is at risk of dying… today. The CDC estimates that more than 100 will in fact die every day. The medical community that unintentionally created this situation by overprescribing opioids now must carry the torch for good and effective treatment. This must be Medication-Assisted Treatment (MAT) – our first line of defense in battling opioid addiction, combined with intensive counseling and outpatient behavioral health services. It can be called cessation or re-adjustment or whatever name makes people feel more comfortable. But it must be done and it must be done without delay. To take a victory lap because less prescriptions are being written is understandable but incomplete as we will find a number of struggling patients who will be forced eventually to rely on heroin before they are ready or able to seek treatment. As a medical community, we shouldn’t be talking about the frequency of prescriptions, without advocating for resources to increase treatment for those who are already addicted to prevent the cost both financial and human in our communities.
Partial truths and story fragments are part of the problem – big picture conversations need to include solutions.
Need help with substance abuse or mentalhealth issues? In the U.S., call 800-662-HELP (4357) for the SAMHSA NationalHelpline.