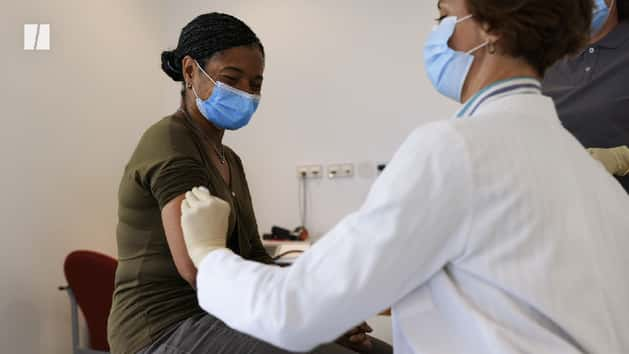
Over the past two years, it’s become more and more difficult to dodge COVID-19, especially as the virus has mutated to become more contagious. We know that high-quality masks help and vaccination drastically reduces our odds of contracting the coronavirus and developing serious illness.
But given the nature of extremely contagious respiratory viruses such as SARS-CoV-2, infectious disease specialists say that most of us will, at some point, get infected. And as the reality of living with endemic COVID sets in, many of us have grown increasingly concerned about getting long COVID if and when that infection occurs.
Because doctors are still researching what causes long COVID in the first place, we don’t have any treatments specifically designed to prevent long COVID. As of now, the best way to prevent a lingering case of COVID — aside from not getting COVID in the first place — is to get vaccinated and start treatment as soon as possible if you do get sick.
“Vaccination and possibly early use of oral antiviral drugs are the most tangible and science-based means to prevent long COVID,” said Richard Becker, an internal medicine physician at the University of Cincinnati College of Medicine who is running the UC Health long COVID clinic.
Where we’re at with understanding what causes and prevents long COVID
Because COVID is a relatively new disease that’s been around for only a couple of years, scientists don’t yet have a solid understanding of what causes long COVID or how to prevent it.
Researchers who study long COVID generally agree that the lingering health effects people experience after their infection are caused by inflammation throughout the body. Others suspect that people with long-haul symptoms still have small amounts of virus in their bodies that may trigger all sorts of health issues, including fatigue, dizziness, brain fog, tremors and chest or joint pain.
We also know that a lot of long COVID patients started out really sick with COVID.
“Just by the nature of being really sick, a lot of patients will have lingering symptoms like fatigue and shortness of breath,” said Jean Paul Higuero-Sevilla, a critical care physician at Yale Medicine who works in the facility’s Post-COVID-19 Recovery Program.
We’re in the early stages of understanding long COVID, and as of now there isn’t a treatment specifically designed to prevent it.
“Figuring out the path of physiology is going to be key to understanding, No. 1, what can be done perhaps to prevent long COVID, and, No. 2, to get us some leads on how to effectively treat long COVID, which currently we don’t really have,” said Sally Hodder, an infectious disease physician and the director of the West Virginia Clinical and Translational Science Institute at West Virginia University.

Vaccination reduces the risk of long COVID
The single most effective way to reduce your risk of long COVID is to avoid getting COVID in the first place. But as infectious disease specialists have told us, that is becoming harder to do as COVID becomes endemic. Remember: Endemic doesn’t mean the virus no longer causes harm, it just means that the harm it does cause is more manageable on a population level. As long as COVID is around, the risk of long COVID isn’t zero.
The best tool to reduce your risk of developing long COVID is to get vaccinated. A study published in January found that vaccination marginally reduced a person’s chances of experiencing long-haul COVID-19. Another report from the United Kingdom found that two doses of a COVID vaccine was associated with a 41% decrease in the odds of reporting long COVID symptoms.
Vaccination reduces your chance of getting COVID in the first place, and, based on this research, also appears to lessen the risk of long COVID, Hodder said. But keep in mind that few studies have been done on this so far. So, though this data is promising, more research is needed, Hodder added. There also have been reports of vaccinated people getting long COVID following a breakthrough case.
Early treatment may help lower your risk, too
If you’re at risk for developing severe disease, you’ll want to start treatment as soon as your first symptoms appear. Evidence has shown that the sicker a person gets with COVID, the higher their risk of it turning into a long COVID case.
Quickly starting the treatments that help keep the infection from worsening may ultimately help reduce your risk of experiencing long-haul symptoms, according to Higuero-Sevilla.
“If you get COVID, especially patients that have co-morbidities, they should talk to their doctor about whether they qualify for monoclonal antibodies or antivirals,” said Higuero-Sevilla, who advises his high-risk patients — including those with diabetes, obesity, heart disease and lung disease — to call him as soon as they schedule a test.
The oral antivirals available to treat COVID should be started within five days of symptom onset. The monoclonal antibody infusion is designed to start within seven days. These medications arrest viral replication and reduce the amount of virus in your body.
“Early diagnosis and treatment with oral antiviral medication or possibly polyclonal antibody may be particularly important for preventing long COVID. This may be the case even for infections producing mild or mild-to-moderate symptoms,” Becker said.
Can over-the-counter medications or rest help?
Knowing that inflammation seems to be at the root of long COVID, you may wonder if over-the-counter anti-inflammatories can help with long-haul symptoms. According to Higuero-Sevilla, there really isn’t any data to suggest that this medication can cut one’s risk of long COVID. We also don’t know if prednisone or dexamethasone — two steroids used to lower inflammation in COVID patients — could affect one’s risk of long COVID, Becker added.
Doctors recommend resting and staying hydrating if you do catch COVID. But whether these interventions will cut your risk of developing long COVID is unknown. That research is ongoing, Hodder said, and if you’d like to participate in studies on long COVID, you can by applying through the National Institutes of Health. Researchers are currently looking for a range of participants — people who’ve had COVID and didn’t get long COVID, people who developed long COVID and people who haven’t been infected — to get a better grasp on what causes long COVID so we can learn how to prevent it.
“It’s going to take a while before we know more about it,” Higuero-Sevilla said. “We don’t have the answers yet.”
Experts are still learning about COVID-19. The information in this story is what was known or available as of publication, but guidance can change as scientists discover more about the virus. Please check the Centers for Disease Control and Prevention for the most updated recommendations.