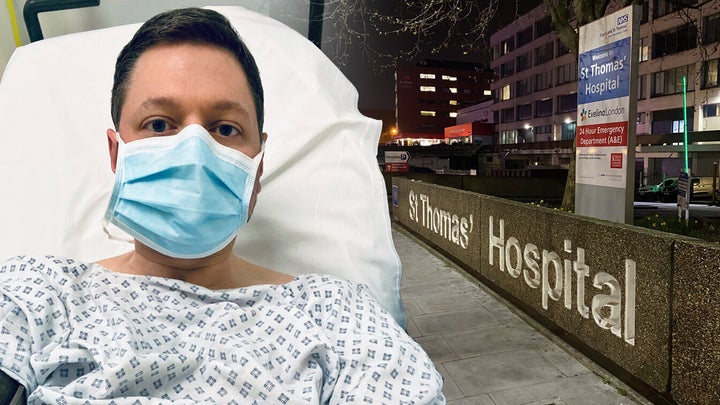
For a growing number of coronavirus patients, recovery hasn’t been swift or easy. In fact, it’s been almost as bad as having the virus itself. I should know — it’s been my daily hell.
Ever since coming down with COVID-19 symptoms in late January, my body feels as though it has been put through the grueling paces of the New York City Marathon without having the proper training for the 26.2-mile run. Or for the tech-savvy, like an iPhone 6S that won’t charge beyond 50 percent.
If I overexert myself, I get a burning, acidic feeling in my lungs, and breathing becomes difficult. A dry cough, along with heart palpitations, come and go. Every muscle and joint aches. If I stand up too quickly, the room gets dark and I nearly pass out.
Electric-like zaps, along with nerve-tingling, radiate throughout my arms, legs and feet. I’m in a constant “brain fog,” always having trouble processing what I’ve just read or heard, or constantly trying to remember familiar names, dates and facts. I have constant pounding headaches that make it extremely difficult to do much of anything. And my dreams — when I can actually get more than three hours of sleep — are intense, bizarre and movie-like.
Welcome to the life of a COVID-19 “long-hauler.” It’s a terrible place to be — a kind of purgatory between being sick and being healed, not having a mild case or a severe-enough one to be on a ventilator in the hospital intensive care unit.
How it all began
So how did this “Dante’s Inferno”-like journey start? It began at Iceland’s iconic geothermal spa the Blue Lagoon on Jan. 18. Five days later, it picked up at Chelsea & Westminster Hospital in London.
After returning home to the U.K. from a long weekend in Reykjavik, I ended up in the emergency room for lung and heart pain. The doctor suspected a blood clot, but that was later ruled out. An EKG of my heart was irregular but not overly concerning to the staff. I asked if it could be the coronavirus; the doctor didn’t even know what I was talking about. After several hours, I was sent home. My diagnosis? A viral infection, pneumonia and pericarditis — inflammation of the lining around the heart. There was nothing I could do other than rest and drink fluids.
Days later, I was back in the hospital as the pain and symptoms had worsened. The EKG was normal this time, but some of my bloodwork came back irregular. I was sent home with naproxen, an over-the-counter anti-inflammatory drug. Over the next few weeks, my condition seemed to get a little better.
And then March came in like an angry lion. It started with flu-like symptoms — fever, nausea, vomiting, dehydration and chills so bad that I was shaking — and quickly progressed into respiratory and cardiovascular distress: shortness of breath, low oxygen levels, lung pain, cough, heart palpitations and pleurisy, inflammation of the tissue surrounding the lung and chest cavity. It felt as though I was having a heart attack every time I shifted positions on the couch.
I contacted the U.K. coronavirus hotline and was able to have nurses come to my home to administer a nasal swab test. The results came back a few days later: undetected. What? How?
In the days following the test, symptoms persisted and new side effects sprang up, impacting my gastrointestinal tract, eyes, liver, kidney and brain. It was as if the virus were ticking off some “to-do” list. It appeared that my immune system was at war.
Dazed (from the lack of oxygen) and confused (by the flip-flopping advice from officials), I went through several weeks of coronavirus waves: pain followed by recovery followed by pain. In that time, I had turned 40, cut my own hair and ended up looking like Pee Wee Herman. I’d dealt with my deaf dog going blind, and — finally — during a visit to the ER, was diagnosed with COVID-19.
The long haul
After the initial infection cleared up in April, new ailments, combined with old symptoms, set in. Now I fear that I will never be the same again.
But I’m not alone; I’m just one of thousands of coronavirus patients speaking out about the long-term effects of this disease. A joint study by Indiana University School of Medicine and the COVID-19 nonprofit Survivor Corps has compiled nearly 100 symptoms, including hair loss, rashes, diarrhea and neurological issues.
“It started with a severe nosebleed,” Stephanie Taylor, 32, who lives in Smethwick, England, told Yahoo News writer David Knowles. “Never had one before. … Then began the nerve pain: burning, pins and needles. Crawling and tingling starting in my hand, and now it’s everywhere, even my head and face.”
“I have been dealing with this for 105 days, and I’m afraid that I’m never going to get back to 100 percent,” Jennica Harris, 33, of Southern California, said in an interview with Yahoo News reporter Suzanne Smalley.
Long-haulers are like the Jan Brady of coronavirus patients — stuck in the middle, constantly fighting to get doctors, governments and even families to pay attention. It’s perhaps why so many support groups have popped up online and on social media.
Things are changing, though.
Medical practices dedicated to helping patients suffering from the COVID-19 aftermath are popping up in the U.K., Italy and the U.S. Dr. Zijian Chen, medical director for the Mt. Sinai Center for Post-COVID Care in New York City, told me that the goal is twofold: treating patients for a variety of ailments and using the research “to treat the patients that we will have in the future.”
Once admitted, patients are evaluated by a team of doctors representing specialties including pulmonology, neurology, cardiology, dermatology, rheumatology and rehabilitation, to name a few. I discovered the center through word-of-mouth and decided to look into it. Right now, it is accepting only test-positive patients, but the goal is to open up the program in the coming weeks to test-negative patients with symptoms, Chen said.
‘Gaslit’
For many long-haulers, going to the doctor can be one big Groundhog Day of disappointment: an exam followed by tests followed by the phrases “the tests show everything is normal” or “you’re likely just going through anxiety or depression.”
It’s been described as “medical gaslighting” — being told you are fine when you know deep down that you truly are not. It makes you wonder if doctors have forgotten the Hippocratic Oath they swore to uphold.
The issue is particularly stark for women and people of color, who face bias in medical treatments, according to various studies.
“[Doctors were] minimizing me as a woman, minimizing me as a Latina,” Albuquerque, N.M., resident Alisa Valdés told NBC News. “Nobody is going to come right out and say that they’re discriminating against you for those reasons. So what do I have to go by? Intuition, instinct, past experience. The attitude of certain providers. The way they look at you. The way they don’t look at you. The way they shrug you off.”
“I have to remind myself I’m not making this up,” Ailsa Court of Portland, Ore., told NBC News. “Everybody is in this state of questioning reality. From the get-go, this country has been gaslit about COVID, and now on an individual level, patients are being gaslit.”
Epidemiologist Paul Garner, who is battling the long-term effects of the coronavirus, has railed against this type of denialism among doctors. “This stuff is real. People are ill. Doctors need to stop diagnosing this as anxiety,” Garner wrote in the British Medical Journal. “We have messed up before; let’s not do it again with long-term COVID-19 illness.”
For Dr. Chen, the key to changing doctors’ attitudes comes down to a very simple tactic.
“What we are doing is we’re having an open mind and that we’re evaluating every patient — looking at what they have and doing our best to treat them,” he said. “The need to really assess the patient and come up with, I think, even new ways to assess patients, new tools that we haven’t used in the past — that’s going to make a difference because this is really a new disease at this point.”
But it’s not just the doctors doing the gaslighting — it can be your friends and family too. For long-haulers, these responses are all too familiar:
“Oh, you’re just tired and mentally stressed like the rest of us going through the pandemic.”
“Maybe you really have mono?”
“I see you posting on Facebook, so you must be fine.”
Looks can be very deceiving, as they say. For most of us, putting on a brave face is all we can do to keep from going crazy.
A co-worker, who asked to remain anonymous because she has not publicly revealed her coronavirus status, told me that friends and family questioning the symptoms “is a very real experience, and I think many don’t realize the impact it can have on patients who are already exhausted.”
“I was physically and emotionally exhausted — so tired, so weak and so afraid of what could happen next,” she added. “With the unpredictable COVID symptom progression, you just never know what that will look like or if you’ll end up in the hospital on a ventilator.”
Scarlet letter ‘C’
I kept my diagnosis secret to nearly everyone except those who absolutely needed to know. But it felt as if I was carrying around an invisible scarlet letter C around my neck. When should I tell people? Was it their business to know?
I also worried that revealing my status would result in stigmas and shaming. During this pandemic, several groups faced egregious other-ism — especially Asian-Americans, who were, and still are, the target of hate-filled COVID racism.
Hannah Hwang, a bank employee in New York City, recounted to Time magazine that a customer told her, “I don’t want to speak to you. You’re Chinese. Please get me somebody else to work with.”
For COVID-19 patients, dispelling myths and enduring stigmas has become almost a second job. “I call it COVID shaming,” the Rev. Shane Harris, president of the People’s Alliance for Justice, told the Los Angeles Times. “It’s a real thing that happens. It happened to me for weeks after my healing. … I had people badgering me about my health status. That’s personal. You don’t have to tell people your health information.”
The decision to reveal what I had been going through changed after I came across an op-ed in the New York Times titled “I’m 26. Coronavirus Sent Me to the Hospital.” Something just clicked inside me. I found a link to the author’s Slack support group and quickly signed up. I soon wasn’t alone anymore.
I encountered others around the world facing the same issues as me. I felt instant relief and a strong sense of community. I told my story to random strangers, and they responded in kind with words of encouragement and a virtual shoulder to cry on. I also connected with a friend of a friend going through a similar situation. Through solidarity I found hope.
As I was coming back from the pharmacy one sunny afternoon in London, I literally saw the writing on the wall — a billboard that read “Community Is Strength.” It was my Oprah aha moment. It made so much sense. Why was I battling this alone?
I decided to officially “come out” as a coronavirus patient to my family, friends and co-workers. For so long, I wanted to keep this to myself and battle it privately, but it dawned on me that what got me through hard times in the past — and what will get me through this — is a strong support network. In other words: community.
My community rallied hard around me — in London, back home in the United States and Italy, and around the world. I felt the love and the prayers and really believe that the positive reinforcement helped give me the strength to go back to work.

The future
With research coming in real time, patients are left wondering what the future holds. There are simply more questions than answers right now: Are these symptoms forever or will they go away? Are organs damaged? Is the immune system compromised? Is this Post Viral Fatigue Syndrome? Chronic Fatigue Syndrome? Dysautonomia? Guillain-Barré syndrome? Are we disabled?
Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases and a member of the White House coronavirus task force, recognizes the plight of long-haulers and admits that much is still unknown.
“We’re starting to see that they do not recover as completely and as quickly as you would like,” Fauci told MSNBC. “How long does it take you to get back to normal? That's an open question. We’re only six months into the outbreak."
For now, I fight on and hope like the rest of you that answers come quickly.
I want my life back.

For the latest coronavirus news and updates, follow along at https://news.yahoo.com/coronavirus. According to experts, people over 60 and those who are immunocompromised continue to be the most at risk. If you have questions, please reference the CDC’s and WHO’s resource guides.
Read more from Yahoo Life
Want lifestyle and wellness news delivered to your inbox? Sign up here for Yahoo Life’s newsletter.
